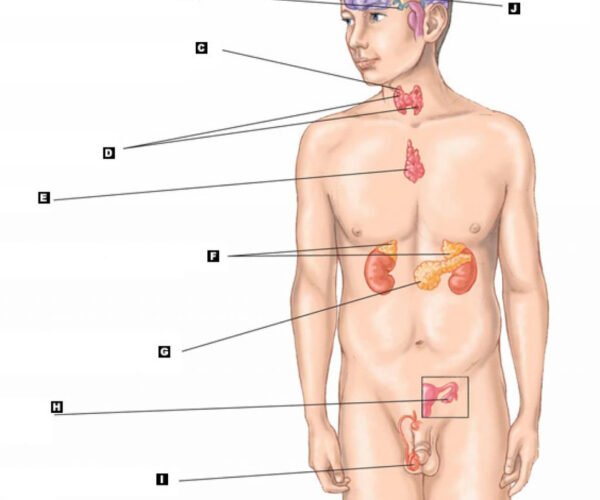
“Testosterone’s Role in Hormonal Disruption: Unraveling the Links to Pituitary Disorders”
Introduction:
Hormonal balance is a delicate symphony orchestrated by various glands in the endocrine system, with the pituitary gland often playing a central role. Among the myriad hormones involved, testosterone, primarily associated with male reproductive health, has emerged as a key player in the intricate web of pituitary disorders. Understanding the interplay between testosterone and pituitary function is crucial for comprehending hormonal disruptions and their impact on overall health.
Testosterone and Its Significance:
Testosterone, the primary male sex hormone, is produced predominantly in the testicles but also in smaller amounts by the adrenal glands. It plays a crucial role in the development of male reproductive tissues, as well as in maintaining muscle mass, bone density, and overall well-being. While testosterone is primarily associated with males, it is present in females in smaller quantities, contributing to their reproductive and general health.
Pituitary Gland: The Master Regulator:
Situated at the base of the brain, the pituitary gland is often referred to as the “master gland” due to its role in regulating the activity of other endocrine glands. It secretes various hormones, including luteinizing hormone (LH) and follicle-stimulating hormone (FSH), which, in turn, stimulate the production of testosterone in the testicles. Any disruption in this finely tuned system can lead to hormonal imbalances and contribute to the development of pituitary disorders.
Testosterone and Pituitary Disorders:
- Hypogonadism: One of the primary connections between testosterone and pituitary disorders is seen in hypogonadism, a condition characterized by low testosterone levels. The pituitary gland plays a pivotal role in regulating testosterone production by releasing LH, which stimulates the testicles to produce testosterone. Dysfunction in the pituitary gland can lead to insufficient LH secretion, resulting in decreased testosterone production and hypogonadism.
- Pituitary Tumors: Pituitary tumors, although usually benign, can cause hormonal disruptions by impacting the production and release of various hormones, including LH and FSH. Depending on the location and size of the tumor, it may interfere with the signals that prompt the testicles to produce testosterone. This disruption can lead to imbalances in testosterone levels, affecting both reproductive and general health.
- Secondary Hypogonadism: Secondary hypogonadism refers to a condition where the problem lies not within the testicles but in the pituitary or hypothalamus. In this scenario, the pituitary gland fails to produce sufficient LH, resulting in decreased stimulation of testosterone production. This form of hypogonadism highlights the intricate relationship between testosterone and pituitary function.
- Prolactinomas: Prolactinomas, tumors that primarily affect the production of prolactin, can indirectly impact testosterone levels. Elevated levels of prolactin can suppress the secretion of GnRH (gonadotropin-releasing hormone), which, in turn, affects the release of LH and FSH. This disruption in the hormonal cascade can ultimately lead to decreased testosterone production.
Treatment Approaches:
Addressing pituitary disorders involving testosterone often requires a comprehensive approach. Depending on the specific condition, treatments may include:
- Hormone Replacement Therapy (HRT): For cases of hypogonadism, especially when related to pituitary dysfunction, hormone replacement therapy may be recommended. This involves administering testosterone to restore normal levels and alleviate symptoms associated with low testosterone.
- Surgery: In cases of pituitary tumors affecting hormonal balance, surgical intervention may be necessary to remove the tumor and restore proper pituitary function. This can be crucial in normalizing testosterone levels and preventing further complications.
- Medication: Certain medications, such as dopamine agonists, may be prescribed to manage prolactinomas and restore hormonal balance. By addressing the underlying cause, these medications can indirectly contribute to maintaining normal testosterone levels.
Conclusion:
The intricate relationship between testosterone and pituitary function highlights the complexity of the endocrine system and the potential for disruption when this delicate balance is disturbed. Understanding the links between testosterone and pituitary disorders is crucial for clinicians in diagnosing and treating these conditions effectively. As research advances, unraveling the mysteries of hormonal disruptions will pave the way for more targeted and personalized interventions, ultimately improving the quality of life for individuals affected by these disorders.
Fertility Frontier: Prostaglandins in Male and Female Reproductive Hormonal Disorders